
(originally published Jan 11, 2012)
Several years ago we became fascinated with the potential of adipose stem cells for both cosmetic and medical purposes. However, we soon discovered that nothing in the written FDA guidelines specifically addressed the use of autologous adipose stem cells.
Thus began our journey for an answer. In June 2009, we sent a letter to the FDA asking for a position statement on adipose stem cells. Our request focused specifically on autologous, freshly isolated, adipose stem cells for use in soft tissue reconstruction. These stem cells are from your own fat, for your own usage, and not culture expanded.
After many FDA conversations and a very long wait, (approximately 2 1/2 years!), we received a written response from the FDA. First, a little bit of background for any stem cell newbies….
Stem cells 101
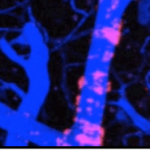
- There are three general categories of stem cells: embryonic, induced pluripotent (IPS), and adult stem cells.
- Stem cell treatments are either autologous or allogeneic. Autologous treatments use your own cells and allogeneic treatments use stem cells from donors.
- Adult autologous stem cells have a higher safety profile than both embryonic and IPS cells.
- Over three thousand clinical trials have taken place worldwide with adult stem cells.
- The adult stem cells in adipose tissue are mesenchymal cells (MSC’s), which are one of the cell types largely responsible for the healing properties of stem cell therapies.
- Compared to other adult stem cell tissue sources, adipose stem cells contain the highest number of healing mesenchymal stem cells (MSCs) per volume of tissue, by a factor of 500 fold. Due to their ease of extraction and highly abundant supply of MSCs, adipose stem cells hold great promise for stem cell therapy.
- Adipose stem cells are derived from fat, which is commonly collected via a liposuction procedure. There are various techniques used to isolate adipose stem cells, but they are generally classified as either freshly isolated or culture expanded.
- The typical method to freshly isolate adipose stem cells combines fat with collagenase to make a stromal vascular fraction (SVF). The process to obtain SVF can be done in a few hours. Culture expansion is used to multiply the number of stem cells and takes days or weeks in a lab.
- SVF is a mixed population of cells containing a high proportion of MSC’s. Culture expanded refers to an SVF population of cells that has been allowed to grow and multiply under specific laboratory conditions. This results in a homogeneous population of MSC’s.
FDA classifications: Tissues vs. drugs
Human cells and tissues intended for human transplant are regulated by the FDA. The FDA maintains two levels of classifications for cells and tissues: 1) HCT/P 361 and 2) HCT/P 351.
uncultured stem cells from my own fat…. a tissue or a drug?
Category 361 is summarized as a ’tissue’ . A subset of category 361 includes procedures that take place in the same operative session . These same session operative procedures are exempt from FDA regulation. These procedures fall under the jurisdiction of practice of medicine.
Surgeons follow guidelines and laws established by state medical boards and their professional societies, but are not controlled by the FDA. The other category, 351, is the ‘drug/biologic’ category, which is completely regulated by the FDA.
It is infinitely easier and faster to bring medical procedures which fall under 361 guidelines to a physician’s practice compared to the 351 category.
Examples of tissues and cell types in each of the two FDA categories are as follows:
- 361-TISSUES: skin, bone, ligaments, corneas, heart valve allographs, hematopoietic stem and progenitor cells derived from peripheral and cord blood, reproductive tissue (IVF procedures)
- 351- DRUGS: prescription drugs, biological products and devices, embryonic stem cells, allogeneic stem cells
Our request simply asked the FDA if SVF (not culture expanded) adipose stem cells for autologous usage in soft tissue reconstruction in the same operative session fall under the tissue or the drug classification.
The FDA response -adipose derived stem cells are a drug
Last month, in December 2011, we finally received a response from the FDA. Close your eyes and imagine a train coming to a screeching halt. It was not the answer we were hoping for.
Your own autologous adipose stem cells from the stromal vascular fraction (SVF) used for reconstruction and repair in the same operative session are considered by the FDA to be a DRUG.
Is the FDA being consistent?
What is interesting to us is that hematopoietic stem cells and IVF procedures are both not classified as drugs, but uncultured fat stem cells are. The FDA’s main consideration for classifying adipose stem cells as a drug was because the cells are more than minimally manipulated. So what about IVF procedures? Is creating a human from a sperm and an egg only a “minimal manipulation”?
What implications does this FDA letter have?
To make a long story short, the ‘drug’ classification will add several years to the equation for surgeons manually performing therapies with adipose stem cells. In our opinion, the FDA’s new position on adipose stem cells will likely have two effects:
- Clinics offering therapies with adipose stem cells will be driven offshore
- In the arms race for adipose stem cells, the power will shift to the device makers specializing in processing adipose tissue.
The new FDA position means that any surgeon who wishes to use the SVF fraction (centrifuged adipose tissue plus collagenase to yield higher numbers of stem cells) must now submit an IND (Investigational New Drug Application) to the FDA and have an approved IRB (Institutional Review Board) with a hospital. This submittal process is extremely time consuming, requires many resources, and is expensive. Some surgeons will simply move their trials, therapies, and clinics offshore.
This FDA position essentially takes surgeons performing manual processing with collagenase in their OR’s out of the physician practice equation for the near future. Therefore, this FDA position likely benefits adipose stem cell device makers who process adipose tissue as they are much further along in the approval process with the FDA. Device makers will likely be first to market with their autologous stem cell processes.
Does this FDA position affect plastic surgeons currently performing high density fat grafting?
No. But it is not out of the question that the FDA may put fat grafting under the magnifying glass in the future.
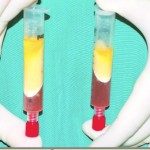
Fat grafting uses fat obtained from liposuction. The fat is harvested with a cannula, decanted, and processed via centrifugation techniques. A portion of the processed fat is then reinjected into areas for cosmetic enhancement. The enhancements primarily involve restoring volume and fullness.
Although fat grafting does not use collagenese to isolate the stem cells, the dirty little secret is that high density fat grafting does contain small numbers of stem cells. These stem cells are found in the ‘fat pellet’ separated via centrifugation after the tumescent liposuction procedure.
The mechanical forces of the liposuction procedure act to separate the mesenchymal stem cells from the blood vessels. This is all within the great science of stem cell activation. Plastic surgeons have recently come to understand that the small population of stem cells in the fat pellet provide more vascularity to fat grafts. High density fat grafting results in long lasting fat grafts and healthier looking skin.




Thomas Wright says:
Dr. Ricardo L Rodriguez says:
Ashley Rafter says:
Pensive Introvert says:
Leeza Rodriguez says:
Leeza Rodriguez says:
Leeza Rodriguez says:
Pensive Introvert says:
Pensive Introvert says:
Pensive Introvert says:
Pensive Introvert says:
Pensive Introvert says:
Leeza Rodriguez says:
Pensive Introvert says:
Brian Sanderson says:
Dr. Ricardo L Rodriguez says:
Brian Sanderson says:
Dr. Ricardo L Rodriguez says:
Leeza Rodriguez says:
Pensive Introvert says:
Dr. Ricardo L Rodriguez says:
Wall Street Titan says:
Dr. Ricardo L Rodriguez says:
Pensive Introvert says:
Dr. Ricardo L Rodriguez says:
Pensive Introvert says:
Dr. Ricardo L Rodriguez says:
Wall Street Titan says:
Dr. Ricardo L Rodriguez says:
Fas Kuiters says:
Dr. Ricardo L Rodriguez says:
Pensive Introvert says:
Pensive Introvert says:
Rosemary Graham-Gardner says:
Dr. Ricardo L Rodriguez says:
Yttevya says: