(originally published on March 4, 2014) History is full of disruptive innovations: Just look at what email did to the postal industry, the Ford Model-T to the transportation industry, and Wikipedia to the traditional encyclopedia. All three of these “disruptive innovations” revolutionized their respective industries via low-cost, democratic solutions.
Luckily, we are at the forefront of an exciting disruption in the healthcare industry via Apple’s upcoming iWatch.

Apple Watch-tracking vital signs is key
On the surface, the iWatch appears to be nothing more than a souped-up version of the Jawbone or FitBit bands. But closer investigation suggests that the iWatch will be somewhat of a portable nurse tracking your vital signs.
According to industry publications, the upcoming iWatch will be able to monitor several body function parameters such as hydration, pulse, and blood pressure.
Further confirming the iWatch’s involvement with healthcare is the fact that a group of senior Apple executives met with the FDA in December 2013 to discuss mobile medical applications.
“Apple noted that while the guidance is a step in the right direction, industry is always going to be pushing the boundaries. Apple sees mobile technology platforms as an opportunity for people to learn more about themselves. With the potential for more sensors on mobile devices, Apple believes there is the opportunity to do more with devices, and that there may be a moral obligation to do more.
Sensors already exist on medical devices. For instance, Apple’s devices have cameras and accelerometers. There is still an opportunity to innovate, but Apple wants to make sure they are on the side of the FDA.“ – Apple and the FDA have discussed FDA regulations regarding possible new mobile products, sensors and a glucometer
Doctors make diagnosis using the clinical picture
The potential impact of the iWatch on the healthcare industry is so exciting because it closes the gap between the “science” and “art” of medicine. This can best be explained by the chronology in which a doctor evaluates, diagnoses, and prescribes treatment for a patient. The “science” of medicine plays the largest role in creating what doctors call the clinical picture, which is comprised of the following two elements:
1. History
The patient history is a recording of the events that led to his or her visit to the doctor. In this case, quantity is as important as quality; even seemingly irrelevant details may be the key to solving this riddle. But patients may not even realize they are experiencing certain symptoms, and doctors don’t always know enough to ask the right questions.
What if there was a way to push a button and get the patient’s entire history?
2. Physical Exam
A patient’s vital signs and body functions are measured through a physical exam at the time of his or her visit. This exam includes readings on elements such as blood pressure, pulse, and temperature. But other subtle signs such as skin moisture, masked anxiety, or subtle color changes in the skin may be missed. In any case, this information is the snapshot of a single point in time: the moment of the physical exam.
What if there was a way to push a button and get a trend-line of the patient’s vital signs and body functions for the past few days, months, or years?
The current clinical picture is incomplete

The “art” of medicine lies in the doctor’s interpretation of a patient’s clinical picture. Each doctor possesses a unique database of knowledge: years of medical school and residency, intuition based on years of experience, and continued learning of current medical literature. With these tools, a doctor prescribes a best course of treatment going forward based on all of this collective knowledge.
But there are two shortcomings in the “art” of medicine.
To begin, the “art” is only as good as the data that precedes it. Not even the best doctor in the world would be able to correctly diagnose and prescribe treatment if working with an inaccurate or incomplete clinical picture.
Second, the immense volume of information in the medical sphere against which a doctor can compare a patient’s clinical picture is far too great for any one person to interpret. Specialization was supposed to solve the problem, but has the unfortunate side effect of fragmented knowledge.
Electronic medical records may help, but they still only represent ‘snapshots’ of the clinical picture when seen by a healthcare professional.
Making the clinical picture more complete
What if there was a way to push a button and get much higher quantity and quality of data that can be processed in real time for the doctor at the moment he needed it for the specific patient?
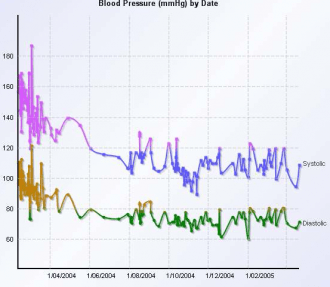
Enter the power that Apple’s iWatch could immediately bring. It would transform the patient’s history into “super history” by presenting all information at the push of a button, including those the doctor never thought to ask or the patient to mention.
The hazy clinical picture now is not only incredibly more detailed, but an iterative trend line of the patient’s progress thus far. The blood pressure would not only be known on the day of the doctor visit, but a doctor could view a trend line from the past few days, weeks, or months.
The simple presence of improved data collection enhances the doctor’s evaluation and diagnosis process tenfold. Sounds exciting? It gets even better. It gets predictive.
The iWatch and big data modeling
The predictive power comes from a data mining tools such as look-alike modeling. In look-alike modeling, patterns of discrete behaviors can be used to predict outcomes. The technique is currently used by web marketers to target ads based on past behavior patterns of customers who are likely to engage in a specific activity. The predictive power of these patterns can also apply to biologic systems.

Your own personal clinical trial
If you think about it, a clinical trial is the creation of such a pattern. You control for the patient’s sex, age, medical condition (i.e. hypertension) and introduce a variable (x or y drug) to see what the response is.
The problem with clinical trials is that there are barriers. They are very resource intensive (money, personnel, regulatory, etc.) and the predictive power applies to only a few patients — those that fulfill the study conditions.
But what if you could have at your fingertips a “personalized clinical trial” based on your patient’s conditions?
Data modeling and the Apple Watch
That is what data modeling can do with the aggregation of all those “super histories.” It can sift through all the data and find those patients whose symptom patterns are similar to yours. From these past “super histories” you can tell how the symptoms are likely to evolve and give you a sense of urgency. Data modeling can also give you an idea what the responses were to x or y medication in patients like the one in front of you.

The process sounds a lot like the “art” part of what a doctor now does by comparing the clinical picture (a pattern of discrete behaviors and physical attributes) of his patient to other clinical pictures he remembers. Except that now the comparison is not to other clinical pictures in the doctor’s memory databank, but to all the real time clinical presentations in the database. And instead of targeting an ad to alter the outcome, you stage a medical intervention.
The intervention may even be preventive, for example if the iWatch detects a dangerous pattern in your heart rate, skin moisture, blood pressure, etc. it may just activate a buzz alarm to tell you to slow down and at the same time alert your primary care doctor.
Looking even further into the future, the iWatch has the opportunity to expand and refine the medical knowledge database because it brings to bear knowledge the medical profession now does not collect. Social media data and GPS data can tie in to the data obtained by the iWatch to infer cohort behavior patterns. This is powerful real time epidemiological data that enhances medical decision making.
How Apple Watch helps my surgical practice

Let me give you an example from my surgical practice.
Consider a patient who had surgery a few days ago and is feeling flush and warm at midnight. She is concerned, but doesn’t know if she should place a phone call to me.
The iWatch reads a pattern of heart rate, skin moisture, and daily fluctuation of temperature consistent with infection. It sends the info back as a red flag and alerts me. Based on the patient’s GPS, it also alerts me of an unusually high number of Staphylococcus infections in the persons area.
You can be sure I’ll call her and ask a lot of questions and, based on her answers, may even prescribe her antibiotics. We interrupt the problem before she even realized there was one, and before it gets worse.
Apple Watch gives information to healthcare providers
For the first time ever, real time vital signs can be collected from millions of people in the general population and aggregated in centralized databases. Doctors and healthcare providers will be able to make quicker and better informed diagnosis. The iWatch will usher in a new healthcare ecosystem with fantastic predictive powers.
The iWatch will be a truly disruptive innovation for Medicine. It democratizes and frees up a not only a crucial body of information — the Enhanced Clinical Presentation and individual responses to therapy — but also the way we collect the information. Say goodbye to snapshot pictures of your health. With the iWatch, you will have a continuous medical chart feed and a glimpse of your health future.
Update July, 2022: Apple released this report which outlines their strategy in the health care markets for both consumers as well as healthcare systems.
Spearheaded by Apple’s chief operating officer, Jeff Williams, the report is the first time Apple has offered a comprehensive view of its approach to healthcare markets in the eight years since it began releasing health features such as a medical records storage system on iPhones. It has also started partnering with institutions such the Stanford University School of Medicine to conduct large-scale formal medical studies.
Much of the work has centered around the Apple Watch, a device that Williams played a key role in bringing to market and which contains sensors for heart health and other functions.
https://nypost.com/2022/07/20/apple-unveils-healthcare-strategy-with-apple-watch-iphone/
(Article originally published on March 4, 2014)



